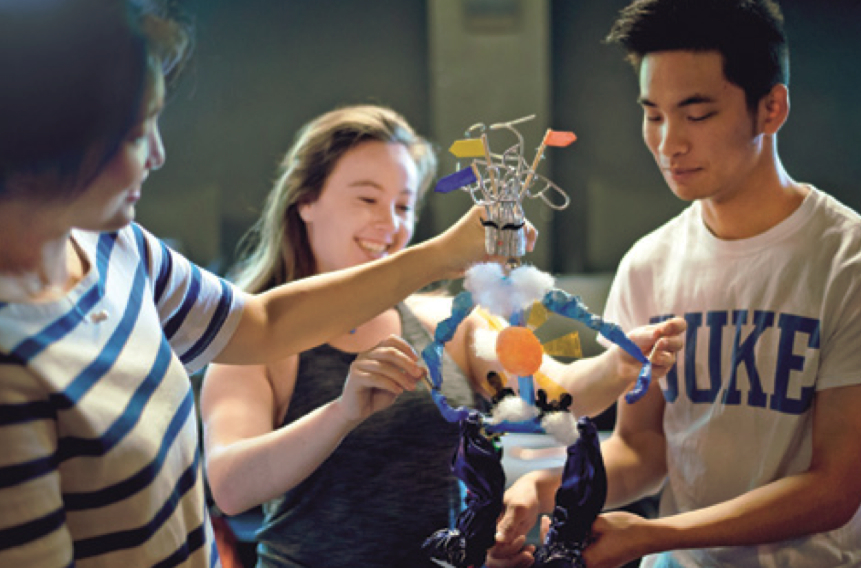SOCIAL JUSTICE
FALL/WINTER ISSUE NO. 44
Table of Contents • Editor's Note • Selections
ATTENDING TO THE “ILLUSION OF LIFE”:
REIMAGINING MEDICINE THROUGH THE ART OF PUPPETRY PRACTICE
by Marina Tsaplina, Jules Odendahl-James and Torry Bend
photos: Robert Zimmerman and Ben Shepard
The pedagogy of suffering is my antidote to administrative systems that cannot take suffering into account because they are abstracted from the needs of bodies. When the body’s vulnerability and pain are kept in the foreground, a new social ethic is required.
–Arthur Frank, The Wounded Storyteller (146)
Puppetry is defined as the manipulation and animation of an object to create the illusion of life.
–UNIMA (Union Internationale de la Marionnette)
The profound questions of life and death that the experience of illness calls to the surface are unable to be understood through the language of biology and capitalism. This is the work of Art and the Humanities, and puppetry and theater artists have an active role to play.
Medicine in the United States is in crisis. There is an epidemic of physician burnout, with 46% of physicians reporting “a physical or mental collapse due to overwork or stress.”1 “Physician heal thyself” has never taken on a more relevant and necessary cry for the safety of patients and the profession as a whole.2 American healthcare continues to be plagued by entrenched racial, gender, and economic inequity. Doctors (a majority male3 and white4) sit at the top of the organizational pyramid, with the remaining members of a healthcare team (e.g., nurses, social workers, physician’s assistants, and a host of other professionals) not to mention the persons-in-care marginalized in their authority. In response, patient and disability communities over the past three decades have organized their voice: strengthening the assertion of one’s own agency in the lived experience of illness5.
Yet can we ask individuals to heal themselves in a system that doesn’t create conditions for flourishing? There is an overarching crisis that impacts all the multifaceted layers of twenty-first century healthcare: the erasure of healthcare provider, caregiver, and patient bodies and voices. The for-profit healthcare industry reduces human beings to biological entities, legal liabilities, dollar signs, and administrative burdens. Physicians, despite their “top of the food chain” status, have become figureheads, their agency constrained by bureaucracy and the “technologization” of medicine’s delivery. Bodies-in-care and diseases become objects to be examined, contained, and categorized according to insurance coding. Additionally, medical education shapes future healthcare providers through engagement with the hard sciences predominantly if not exclusively, forming a mechanical view of the body.
In the summer of 2018, the authors created a ten session module titled, “Puppetry and Embodied Imagination” for pre-health undergraduate students at Duke University as part of a new program: Reimagining Medicine. As home to one of the top ten medical schools in the United States, half of Duke’s incoming undergraduate class plan to pursue pre-health coursework.
The brainchild of pediatric oncologist and writer Dr. Raymond Barfield, Reimagining Medicine’s goals are to foster the strength of character, practices, and philosophical foundations needed to work in contexts of human suffering, loss, and death.
The centrality of the arts to this endeavor is exemplified by Dr. Barfield’s collaboration with puppetry artist and patient activist Marina Tsaplina in the formation of the program. Inclusion of puppetry was the central vehicle for exploring not just creative imagination or storytelling but embodiment itself, embodiment as evolving and collaborative within the contexts of the experience, diagnosis, and treatment of illness.
We engaged in a discovery of how puppetry’s practices cultivate presence, attention, and imagination. These three dimensions engage future healthcare providers in a practice that holds healing at its core. These dimensions are being extinguished in healthcare, leading to the vocational crisis and violations of human dignity cited at the opening of this article.
FORM AS CONTENT
Creating the “illusion of life” in puppetry demands a contract between puppeteer and audience. A puppet is a material site of pure imagination, where the artist sets up the rules of play in anticipation of an audience’s recognition of the object’s behavior, its “life.” When the illusion is successful, the “object” becomes a “subject” that is able to hold and expand the audience’s relationship to it. It is this identification that leads to responses of profound beauty, sorrow, laughter, and joy in puppet theater. When its poetic capabilities are invoked over narrative specificity, the same story can hold multiple interpretations.
We found three purposes in the limited medical scholarly literature6 on puppetry’s use in healthcare:
to convey health or medication information to patients;
to teach empathy or interpersonal skills to healthcare professionals or students or
to fill in representational gaps, particularly about individuals with disabilities, in the telling of stories about illness for patient groups and the larger public.
Such materials detail a use of puppets within medical contexts focused on messaging and explanation – the “illusion of life” provided by the puppet/object strives for shared meaning and purpose above all. Puppetry in medicine effectively includes bodies and stories too often left out of diagnostic narratives.
However, as puppetry artists/scholars Purcell-Gates and Fisher argue, “puppets, as bodies that are materially constructed, can both reinforce and rupture [cultural] constructions [of the disabled body].”7 Similarly, we were resolute in our conviction that we should not offer the predominantly able-bodied students of Reimagining Medicine an “illusion” of a life of illness, where the object/puppet is a mechanism by which to perform disability. Instead, we hypothesized that focusing on puppetry’s intrinsic construction of the illusion of life, essentially peeling back the layers of the art form itself, would offer ways to perceive body and being as a process. Instead of a puppet being directly representational of “patient with condition X,” we asked students to engage with a body/being on its own terms. This brought into question fundamental notions of what it means to be a body in the world at all.
Such a hypothesis required us to articulate the dimensions of an “illusion of life” within the clinical encounter. In that context, the person-in-care possesses a life that has been disrupted or complicated by medical need. Within the doctor’s visit there is a similar artist/audience contract being negotiated between patient and physician where the question arises: Who sets the boundaries of this world?
Medical sociologist Arthur Frank argues the testimony of the patient is not simply an account of the things that are happening/have happened, e.g. a report of unquenchable thirst, which may be a symptom of elevated blood sugar in diabetes. Rather, illness stories are told by “witnesses [who] are what they testify.”8 Illness stories are stories of being as well as stories about being. Similarly in puppetry, one must negotiate material objects in tactile ways that offer a unique realm of experience. Objects have their own demands. The process of puppet/object manipulation offers a kind of direct access to the struggle over definition and being present in the clinical encounter. The goal is for all members to arrive at a shared definition of the patients’ lived conditions based on representations of symptoms, “illusions of life.”
POETIC BODY
We did not begin our unit with puppets, but with the students’ own bodies. The cumulative eighteen-hour workshop series wove together a tapestry of exercises pulled from diverse theatrical pedagogies that hold the body at the center: Margolis Method, Linklater, Pochinko Clown, Action Theater Improvisation, and Sandglass Theater.
The assertion was that presence and attention are vehicles of imagination that cultivate an awareness of personal embodiment through which students begin understanding the story (the testimony) of their own bodies and the bodies of others. The work focused on practices in relation and tension within self and between self and others, locating imagination within and through the body: the body personal and collective, human and puppet, social and historic.
After three and a half days of embodied practice, we introduced simple foam-ball-and-rod puppets, modeled off the training forms of Sandglass Theater. The students’ practice was to stay in breath and connection with this object, as they worked their imaginative reach to “see” through it and find its response to stimuli. A simple story-pattern was offered: Enter, breathe, see something, respond, exit.
Puppetry as a form renders presence palpably visible: there is no hiding. Those students who struggled the most to come into presence and connect to their own bodies treated the puppets as mere sticks with balls, passing quickly through a rather mechanized enactment of the story-pattern. Others created more elaborate scenarios, eager to evoke the amusement of the audience. They were steered back to breath by the directive “build with more attention not action.”
We then introduced a series of multi-person puppets, with leather snap-joints based on the design of Hansjürgen Fettig. Finding the new realities that emerged from switching puppet body parts illuminated the nature of illness/disability, asking each group of “puppeteers” to find the forms’ new ground of being, questioning the idea of “normal” and “baseline.” The use of snap-joints was not an anatomical “trick” but rather exposed anatomical function. The healthy body is presumed given and transparent, until it somehow doesn’t “work” anymore, and its constructs become visible. Thus the “story” became moving from one set of coherences to another, finding the life of this amalgamation of forms.
One set of these snap-joint puppets came from the students own visualizations, following a movement-meditation that generated imagery that emerged from the body. These visualizations were built by Torry Bend and Marina Tsaplina into a collection of design-gestures: individual puppet body parts that were then composed into four puppets. This now brought the personal imagined experience each student had into palpable form that existed in relationship with other students’ embodied imaginations. These puppets became negotiations of a collective imagination, pushing and pulling individual meaning into a coherent whole that, because of the presence of the snap-joints, always carried the possibility of being disrupted again.
(W)HOLISTIC MEDICINE
Each clinical encounter requires delicate negotiations over the definition of reality, between what a healthcare professional tells the person-in-care about condition X, and what that person understands and experiences of condition X. This negotiation between the person-in-care and the physician becomes newly visible in puppetry. For Reimagining Medicine, it is this more complex understanding of illness that is productive for pre-health students. In our puppetry unit, the scientific materiality of the body that students learn through chemistry and biology is now met with metaphoric understanding. Breath/vocal work, clowning exercises, and puppetry work (albeit nascent) cultivate poetic materiality, an integration of how breath, body, voice, emotion, thought and imagination create meaning. This new perspective on materiality was not necessarily in the service of a medical narrative (e.g. using puppets to enact stories of empathy between doctor and patient). Instead, we used puppetry to emphasize structures of being (alone and in relation) that were abstract and fragile even in their uncompromising materiality. We pressed students to ask: What is in this object in front of me? How does it want to move and be? The goal was to illuminate the unique ways objects speak and negotiate through their own physical demands, beyond language, making manifest dynamics that are found in clinical encounters.
We asked students to focus on embodiment stripped of overt healthcare context. The puppets didn’t have wheelchairs or IV tubes; these were not overtly suffering bodies. Instead, students spent time considering their own involuntary and voluntary breath, producing collective action without words, and moving a puppet “body” from one place to another, manipulating that object outside of but in concert with their own bodies. These practices offered them an incremental, iterative consciousness of being a body in the world. They did not engage objects to tell stories about being but to create a coming into being. A critical intervention in healthcare delivery with social justice at its foundation is this: fostering a cultivated attention to the human being in front of you as the human being that you are.
The practice of a disembodied medicine has produced a crisis in twenty-first century healthcare. Our focus on puppetry and physical theater practice as medical humanities research technique is unique to Reimagining Medicine. In the closing circle of our sessions, one student said: “What I am carrying away with me is that wholeness does not mean there is no brokenness.” We are encouraged that such a consciousness in a prospective physician marks our work’s potential to heal some of the personal, social, and civic fractures in the body of medicine.
MARINA TSAPLINA is a puppetry artist and scholar working in the field of the medical/health humanities. She is an Associate of the Trent Center for Bioethics, Humanities and History of Medicine at Duke University where she serves as co-director of Reimagining Medicine. As a patient activist, she is part of the #insulin4all movement for affordable medicines in the United States. Her current interdisciplinary puppetry project is Illness Revelations: The Bodies of Medicine.
JULES ODENDAHL-JAMES, Ph.D, MFA is a professional dramaturg and director. She is an adjunct lecturer in Theater Studies at Duke University where she also serves as the Director of Academic Engagement for the Arts and Humanities. Most recently a Kienle Scholar in Medical Humanities at Penn State College of Medicine (2016-2018), she specializes in work by women playwrights; developing new collaborations across the arts and the sciences; and creating performances about science and medicine.
Puppetry artist and scenic designer TORRY BEND was a collaborator and faculty on Puppetry and Embodied Imagination. She currently serves as Department Chair of Theater Studies at Duke University.
Endnotes
1 https://www.medscape.com/viewarticle/774827
2 https://catalyst.nejm.org/physician-well-being-efficiency-wellness-resilience/
3 https://www.theguardian.com/commentisfree/2018/jan/14/why-are-there-still-so-few-female-doctors
4 https://news.vice.com/article/why-are-there-so-few-minority-doctors-united-states
5 We use “illness,” “disability,” and “condition” interchangeably, as it is beyond the scope of this article to articulate the nuances of apparent/non-apparent disabilities, chronic vs. acute conditions, and interconnections between physical and mental health. We are discussing health in the broadest sense of the term.
6 Some examples, “Using puppetry to elicit children’s talk for research,” Nursing Inquiry (2008); “A review of the literature – The use of interactive puppet simulation in nursing education and children’s healthcare,” Nurse Education in Practice (2017); “Using Puppets to Teach Schoolchildren to Detect Stroke and Call 911,” Journal of School Nursing (2016). See also Tsaplina’s work in THE BETES Organization.
7 “Puppetry as reinforcement or rupture of cultural perceptions of the disabled body,” Research in Drama Education: The Journal of Applied Theatre and Performance (2017).
8 The Wounded Storyteller: Body, Illness, and Ethics second edition. 140.